The main causes of premature mortality are gendered
Life expectancy at birth is defined as how long a newborn can expect to live, on average, if current death rates do not change. As a main indicator of human longevity, life expectancy is often used to characterise the health status of a population (Johnson et al., 2020). On average, women in the EU are expected to live until 84 years of age, which is 5.5 years more than men, at 78.5 years. However, this figure varies substantially between countries[1] (Franklin et al., 2021; OECD/European Union, 2020).
As mentioned in the domain of health chapter (see Chapter 7), COVID-19 has negatively affected life expectancy in most EU countries, particularly for men.
The gender gap in life expectancy is often attributed to a combination of biology and modifiable factors, such as risky behaviour, smoking and excessive alcohol consumption (Kolip, 2012; Stephens et al., 2017), as well as the different societal roles of women and men (Hoffmann et al., 2018). Men’s lower life expectancy reflects their thinking on masculinity and way of life, which determines their exposure to risk, their health-seeking behaviours and how health providers address men and their health needs (WHO Regional Office for Europe, 2018).
Education – one of the most documented social determinants of life expectancy – is used to measure the impact of social and economic status on longevity. Here, too, men are particularly affected. The OECD found that the average difference in life expectancy among 30-year-old men between those without an upper secondary education and those with a tertiary education was 7 years. The impact of education is particularly notable – amounting to a difference of 10 years – in Hungary, Poland and Slovakia (OECD/European Union, 2020). Similarly, studies show that women educated to tertiary level live longer than those with lower qualifications (WHO, 2016d). For example, Roma women have a shorter life expectancy than women in the population at large (EPHA, 2018).
Such gender differences are reflected in data on causes of premature mortality in EU countries. Men are more likely than women to die from causes related to risky health behaviour. According to Global Burden of Disease (GBD) 2019 data[2], the rate of premature mortality[3] from external causes, such as accidents, suicides, injuries, homicides and other violent deaths, is higher among men (10 %) than among women (5 %).
The main causes of premature death among adults also affect women and men to different degrees (Table 3). For example, while cardiovascular diseases and strokes are the principal causes of death for both women and men, many more men than women die from ischaemic heart disease (+ 31 p.p.). As WHO notes, such diseases are perceived as men’s issues, with health systems tending to minimise or overlook risk factors in women (WHO, 2016d).
Among other common causes of premature death for men are liver disease and suicide – ranking sixth and seventh, respectively. Alzheimer’s disease and other dementias, as well as hypertensive heart disease, are among the most common causes for women – ranking fifth and ninth, respectively. Sex-specific cancers similarly lead to significant early loss of life among women and men. Breast cancer is the third highest-ranking cause of premature death for women, while prostate cancer ranks eighth for men.
Table 3. Leading causes of premature mortality among women and men (number of years of life lost, 20+ years, EU, 2019)
| Cause | Women | Men | Gender gap (p.p.) |
|---|---|---|---|
|
Ischaemic heart disease |
5 406 350 |
7 832 577 |
31 |
|
Stroke |
3 613 705 |
3 315 024 |
– 9 |
|
Tracheal, bronchus and lung cancer |
2 114 608 |
4 545 089 |
53 |
|
Colon and rectum cancer |
1 541 334 |
2 079 668 |
26 |
|
Chronic obstructive pulmonary disease |
1 293 433 |
1 945 706 |
34 |
|
Alzheimer’s disease and other dementias |
1 918 196 |
978 477 |
– 96 |
|
Cirrhosis and other chronic liver diseases |
832 997 |
1 839 797 |
55 |
|
Self-harm |
496 962 |
1 801 050 |
72 |
|
Lower respiratory tract infections |
1 036 074 |
1 244 853 |
17 |
|
Pancreatic cancer |
932 009 |
1 090 042 |
14 |
|
Diabetes mellitus |
771 538 |
868 921 |
11 |
|
Chronic kidney disease |
760 603 |
737 302 |
– 3 |
|
Stomach cancer |
529 536 |
894 968 |
41 |
|
Sex-specific cancers |
|||
|
Prostate cancer |
|
1 500 678 |
|
|
Breast cancer |
2 276 349 |
|
|
|
Ovarian cancer |
768 439 |
|
|
Source: Number of years of life lost, 2019, GBD. Authors’ calculations.
Data from the European Cancer Information System shows that in 2020 more men than women were diagnosed with cancer, with men accounting for 54 % of cancer diagnoses in that year (and women 46 %). Most new cases among men are lung, colorectal and prostate cancer. For women, breast cancer is the most prevalent, at 29 %, followed by colorectal cancer at 12 %, and lung cancer at 9 % (OECD/European Union, 2020).
Gender differences in death associated with mental health, such as dementia, suicide and alcohol and drug abuse, are particularly stark. For example, in 2018, the rate of mortality from overdoses among people aged between 15 and 64 years was 22.3 per million, but the rate was almost four times higher among men than among women. Men aged between 35 and 44 years were most affected, with a mortality rate of 53.7 deaths per million. This is more than double the average for all ages, and more than three times the rate of mortality from overdose of women in the same age group, which was 13.9 deaths per million (European Monitoring Centre for Drugs and Drug Addiction, 2020).
Eurostat’s mortality data on suicide and mental and behavioural disorders, including deaths from alcohol and drug abuse, also reveals that more men than women die from these causes (Figure 27)[4].
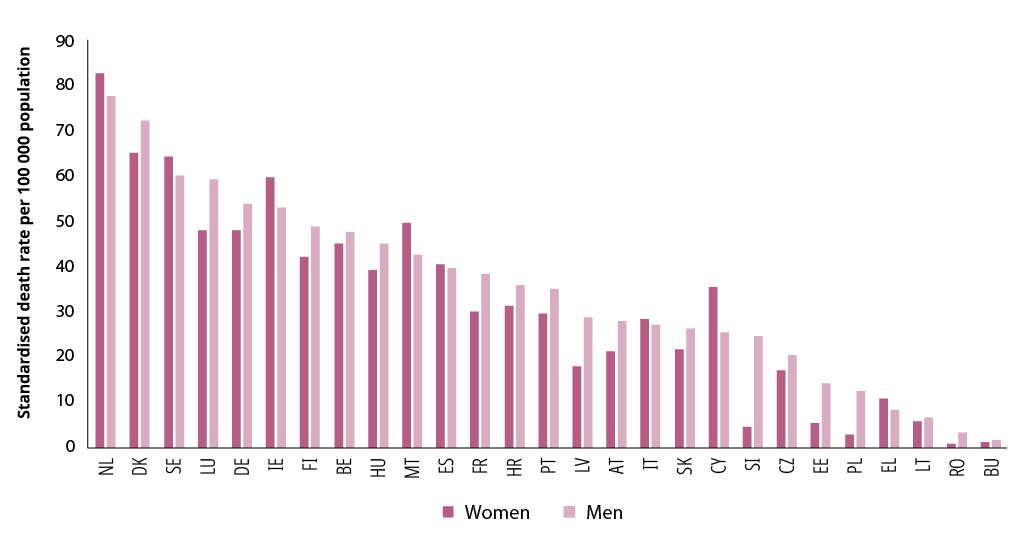
Only in eight countries – Cyprus, Greece, Ireland, Italy, Malta, Netherlands, Spain and Sweden – do more women than men die of mental and behavioural disorders. This can be attributed to the high prevalence of Alzheimer’s disease and other dementias among women. In those countries where mortality from mental and behavioural disorders is higher among men, the difference is mainly due to a large gender gap in deaths from alcohol-related causes.
A systematic review highlights that men are more likely than women to die from suicide, although more young women than young men attempt suicide (Miranda-Mendizabal et al., 2019)[5]. Gender differences in suicide are large, especially in central and eastern Europe. Here, the age-standardised mortality rate for suicide is five times higher for men than for women. In western Europe, it is 3.3 times higher for men than for women (Naghavi, 2019).
Figure 27. Death rate of women and men due to mental and behavioural disorders, by EU Member State (% per 100 000 population, 2014–2017 average rate)
NB: EU-27 average not available. Mental and behavioural disorders include dementia and mental and behavioural disorders due to use of alcohol, drug dependence and toxicomania, as well as other mental and behavioural disorders.
Source: Eurostat, https://ec.europa.eu/eurostat/web/products-datasets/-/hlth_cd_asdr2.
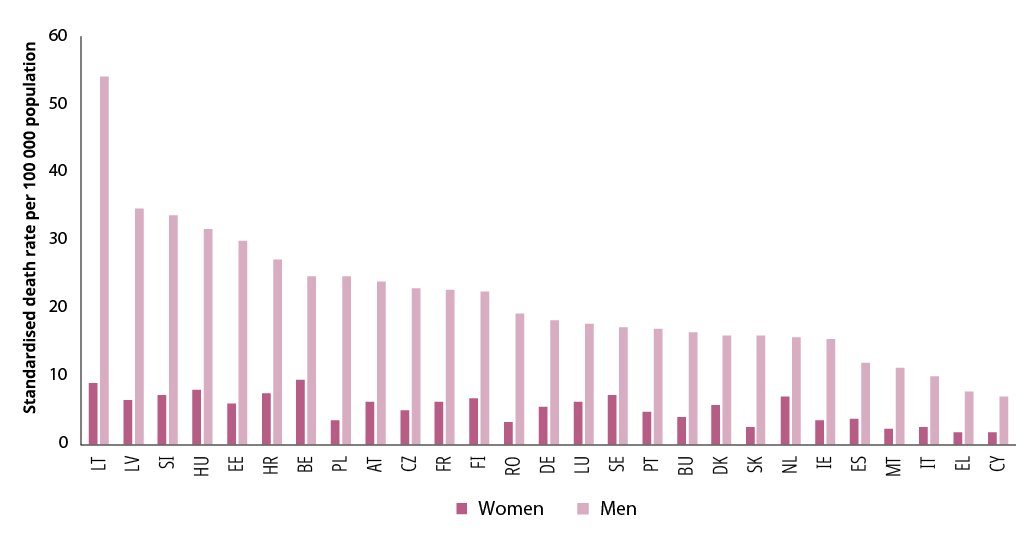
Figure 28. Death rate of women and men due to intentional self-harm, by EU Member State (% per 100 000 population, 2014–2017 average rate)
NB: EU-27 average not available.
Source: Eurostat, https://ec.europa.eu/eurostat/web/products-datasets/-/hlth_cd_asdr2.
Similarly, deaths from intentional self-harm are far more prevalent among men than women in all EU countries (Figure 28). The variations in suicide rates between countries are particularly large among men, while differences among women are much smaller. Gender differences in deaths from self-harm are particularly evident in central and eastern Europe.