
While women and men make up an equal share of those infected with Covid-19, men are more likely to die from the disease. [1] Biologically, this could be because females tend to have stronger immune responses. However, other factors may also be at play, including gender differences in behaviour that affects health, such as smoking.
While women have a longer life expectancy than men, they spend less years living in good health. Due to a higher life expectancy and higher likelihood of facing health problems (see graph below), women are more likely to be in need of long-term care.
This is now further complicated as older people, and especially women who are living alone and depend on care from family, friends or neighbours will no longer be able to rely on it to the same extent. For older people living in residential facilities, social distancing measures can increase their chances of social exclusion as visitors are denied entry.
Women and men limited in their usual activities due to health problems, by age group and level of difficulty experienced (%, EU-28, 2018)
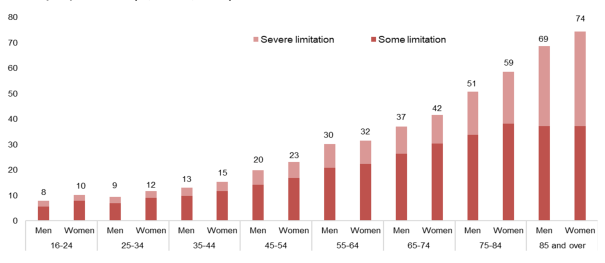
Note: Data labels refer to the total percentage of women and men of each group reporting some or severe health limitations
As vaccines against Covid-19 begin to be rolled out, it’s important to collect sex-disaggregated data on the different responses of women and men. This can include the different responses of groups undergoing hormonal therapies, either after menopause or to align their physical appearance with their gender identity. Clinical trials for new vaccines must include a gender-balanced representation of women to see how the vaccine might affect women and men differently.
Medical research has historically shown limited gender sensitivity but an important step forward in this respect has been the Clinical Trials Regulation of the European Commission (2014). It requires the consideration of gender in clinical trials. It should help address concerns about drugs being mainly tested on men, which can mask adverse side effects that are more common among or exclusive to women.
Insufficient gender sensitivity in medical research and healthcare is perhaps not very surprising, given the under-representation of women in health governance and decision-making. Although women are well represented among medical students and doctors, they are less well represented among senior doctors and professors, or in executive health sector positions overall [2].
An examination of 115 Covid-19 decision-making and expert task forces across 87 countries found that in 85 % the majority of members are men.
In 2021, EIGE’s Gender Equality Index will have a special focus on health. It will look into the gender impacts of the Covid-19 pandemic. It will also look at which groups of women and men are the most vulnerable during these situations, and will explore policy measures that can best tackle these inequalities.
What policymakers need to know
- Recognising the different extent to which disease outbreaks affect women and men is a fundamental step to understand the effects of a health emergency on different individuals and communities, and to create effective, equitable policies and interventions. [3]
- Experience from past pandemic outbreaks show the importance of incorporating gender analysis into the preparedness and institutional response to improve the effectiveness of health interventions and promote gender and health equity goals. [4]
- Medical research and health services that address the impact of both sex (biological factors) and gender (social factors) on the health differences of women and men would help to better serve their individual health needs.
- Increasing the representation of women in health governance, decision-making and certain occupations (e.g. senior doctors, professors or researchers) could help to ensure that women also have an opportunity to shape important healthcare decisions
For more information
Gender mainstreaming in health
Gender Equality Index 2020 – domain of health
Coronavirus pandemic: Impact on gender equality (factsheet from the European Commission)