Women report poorer mental well-being than men

Mental health is defined as the state of well-being in which individuals can realise their own potential, cope with the normal stresses of life, work productively and contribute to their community (WHO, 2018a). Mental health disorders refer to a wide range of conditions affecting mood, thinking, behaviour and relationships with others. With the COVID-19 pandemic posing an unprecedented challenge to collective mental well-being, mental health issues could hamper recovery if they are not addressed.
Understanding how poor mental health affects women and men, and the role that gender norms and relations play in shaping it, can help improve overall health status in the EU. The following sections give an overview of gender differences in mental health over the life course and explore how gender contributes to shaping mental health.
Developed in 1998 by the WHO Regional Office in Europe, the WHO-5[1] measures current mental well-being. It is considered a valid tool for measuring mental health and screening depression in various populations (Topp et al., 2015; WHO, 1998).
Analysis of the WHO-5 2016 – where a score of 100 represents the best imaginable well-being, while scores of 50 or lower indicate risk of depression – shows that the self-rated mental health index among those over 18 is slightly higher for men than for women.
The average score in Europe is 66 points for men and 62 points for women. Women, as well as showing lower levels of mental well-being (Dreger et al., 2016), are significantly more likely to report feeling unhappy, depressed unable to overcome problems and a loss of self-confidence (Olafsdottir, 2017).
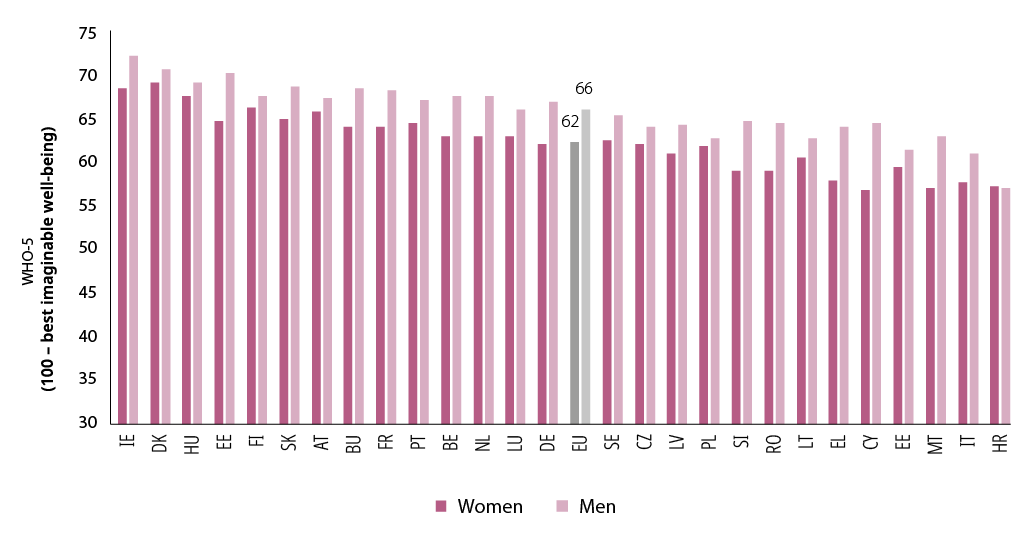
Mental well-being varies across European countries. It is highest for men in Ireland and Denmark, at above 70 points, and lowest in Croatia and Italy, at below 60 points. Although there are clear differences between Member States in self-rated mental well-being, gender differences are small, with an average gap of 4 points (Figure 29).
Figure 29. Self-rated mental well-being of women and men according to the WHO-5, by EU Member State (points out of 100, 18+ years, 2016)
Source: EQLS, 2016. Countries are sorted by their overall WHO-5 scores.
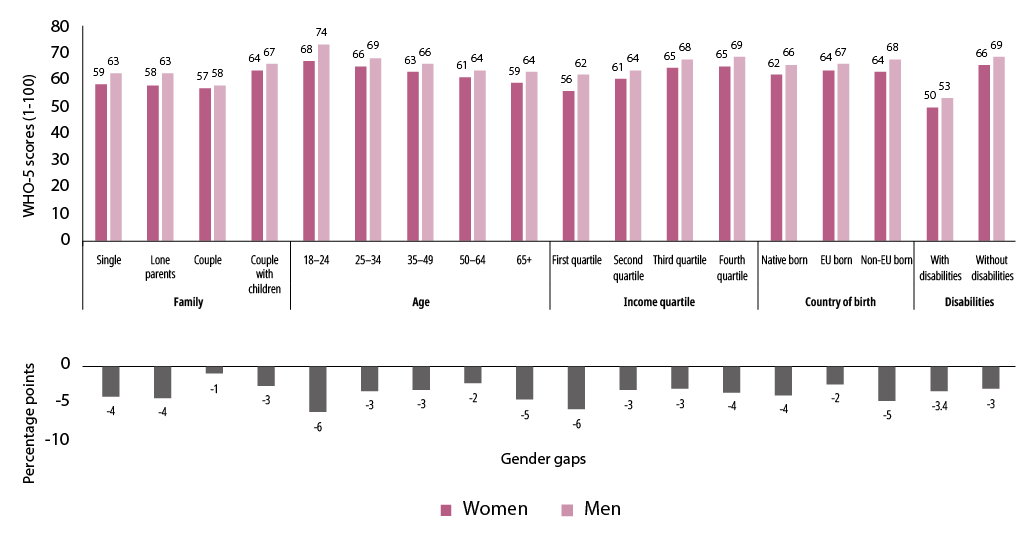
Figure 30. Self-rated mental well-being of women and men according to the WHO-5, by sex, family composition, age, income level, country of birth and disability status (points out of 100, 18+ years, EU, 2016)
Source: Authors’ calculations, EQLS, 2016.
Analysis of self-assessed mental well-being across population groups (Figure 30) shows that women report lower levels of mental well-being regardless of family composition, age, income level, country of birth or disability. Further assessment of levels and gender gaps indicates that social determinants of mental health are potentially at play.
Family structure can also impact mental health. (Figure 30). Caregiving is an important factor influencing the physical and mental health of those providing care, who experience accumulated chronic stressors and often neglect their own health (Young et al., 2020).
Research in Europe shows that being a lone mother or father has a substantial effect on depressive symptoms, regardless of gender (Niedzwiedz et al., 2016) . Similar results have been found in other studies, with single parents suffering worse mental health than couples with children (Chiu et al., 2017; Wade et al., 2011). However, single parenthood can affect the health of mothers and fathers differently. One study found mortality from all causes to be higher among lone fathers (Chiu et al., 2018) while another found that lone mothers had worse mental health than other parents (Collings et al., 2014).
While lone parents are generally agreed to be at increased risk of mental health problems, the combined impact of family structure and gender on mental health can depend on the country and its welfare environment (Niedzwiedz et al., 2016; Palència et al., 2017). On average in the EU, lone mothers report poorer mental well-being than lone fathers (Figure 30). As women are far more likely to be lone parents than men, poor mental health and other single-parent challenges affect a larger proportion of mothers than fathers.
Self-assessed mental health declines with age for both women and men, but is lower for women in all age groups. The gender gap for good mental health is highest among young adults aged 18–24 years, with men scoring 74 points and women 68 points. The gap is lower among those aged 25–64 years, rising again in retirement (Figure 30). Girls are also more likely to self-report lower levels of life satisfaction (Currie, 2016; Inchley et al., 2020). Data from the Health Behaviour in School-aged Children (HBSC) survey reveals that 63 % of boys aged 11–15 years in the EU are satisfied with their life, compared with 56 % of same-age girls[2] . Similarly, girls of this age are much more likely than boys to report multiple health complaints – 44 % and 29 %, respectively – possibly indicating higher levels of somatisation among girls[3].
Women and men with a higher income have better well-being than those with a lower income. Data shows that income increase affects the mental well-being of women slightly more than it does men. The difference in women’s mental well-being index score between the lowest and highest income groups is 9 points. For men, it is 7 points. The gender gap is highest in the lowest income quartile, reiterating how women’s mental health suffers more when their socioeconomic status is low. The same data set also indicates similar findings for education, although gender differences are lower. There is an 8-point difference in women’s mental well-being between those with the lowest and those with the highest levels of education; for men, the difference is 6 points. However, men tend to benefit slightly more in terms of mental well-being when moving from unemployment to employment – by 7 points, compared with 6 points for women. While the findings mirror the analysis of self-reported health, it is important to note that these differences are small and more data is needed to explore these relationships further. Generally, research evidence confirms that social exclusion and material deprivation are the strongest social determinants of poor mental health (Dreger et al., 2014).
Despite limited available data, mental health has clearly and significantly suffered during the pandemic, as discussed in Section 9.2.2.